Maybe let’s start with the fact that the phrase “new private oncology center in London” sounds a bit like a Google search, doesn’t it? Someone in Poland panics after a diagnosis, types those words in, and ends up at Cleveland Clinic London. The problem is, that description is… well, incomplete. The hospital is indeed new, private, and treats cancer — but calling it a specialized oncology center is like calling a supermarket a “bread shop.” Sure, they have bread, but they sell everything else, too.
Cleveland Clinic in London – why does it spark so much excitement?
Cleveland Clinic is a brand from Ohio that has maintained its position among the world’s top hospitals for years. Their model—what Americans call “group practice”—is based on teams of specialists working together, rather than a system of private offices. Expansion began earlier: Cleveland Clinic Abu Dhabi in 2015, then Canada. London was a natural next step—the UK market, especially the private sector, attracts patients from all over the world.
Here’s how it unfolded chronologically:
| Date | Event |
|---|---|
| 2019 | Official announcement of entry into the UK market |
| 09.2021 | Opening of Cleveland Clinic Portland Place – outpatient center |
| 30/03/2022 | Opening of a full hospital at 33 Grosvenor Place |
| 2023 | Full integration of oncology services into the hospital structure |
| 2024-2025 | Development of new programs and specializations |
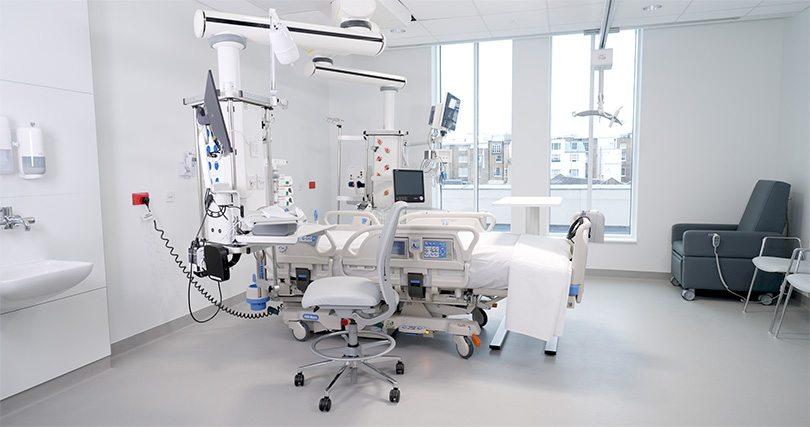
The hospital is literally a stone’s throw from Buckingham Palace – the Grosvenor Place address sounds elegant because it’s one of the most exclusive neighborhoods. Inside, you’ll find several dozen beds (exact numbers aren’t publicly confirmed, but estimates range from about 50 to 80) and an atmosphere that feels more like a boutique hotel than a British NHS facility.
Key departments include:
- Cardiology and cardiac surgery
- Neurology and neurosurgery
- Orthopedics and sports medicine
- Gastroenterology
- Oncology (radiology, chemotherapy, cancer surgery)
As you can see, oncology is part of the portfolio, but it doesn’t dominate. The model is based on self-paying patients or those with international insurance—this isn’t the NHS, so you need either a policy or a willingness to pay out of pocket.

Cleveland Clinic London is a premium, multispecialty academic hospital—it is not a dedicated oncology center. This hospital treats patients with heart issues, neurological conditions, joint problems, and yes—cancer as well. Imagine coming in with lung cancer and also suffering from heart failure. Here, a cardiologist and an oncologist can meet in the hallway. This integration of specialties is something that smaller, oncology-only clinics often lack.
So when someone writes “new oncology center,” they’re not technically lying—but they’re leaving out the bigger picture. In the next section, I’ll show you exactly what cancer care looks like here, because that’s a completely different story.
Oncological care in practice – what does the London hospital offer
A typical Monday in the oncology department at Cleveland Clinic London begins with the entire team gathering over coffee—surgeons, oncologists, radiologists, and pathologists. Every case is discussed; there’s no such thing as “one doctor decides.” This is the moment when everyone looks at the results together and considers the next steps.
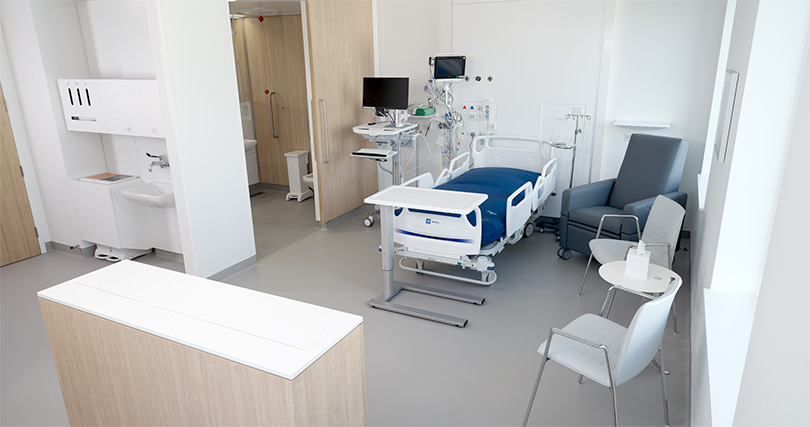
Scope of cancers
The hospital focuses on several main types of cancer. Breast, lung, and prostate cancer are the core areas, but also gastrointestinal, colorectal, and pancreatic cancers. Oncology is one of the key specialties at this facility, though certainly not the only one. Its multidisciplinary nature offers something that smaller centers often lack—immediate access to cardiologists or nephrologists if a patient has additional conditions. After all, no one has just one illness, right?
Technologies and diagnostics
Now, let’s get specific—what’s inside. This isn’t your typical ’90s gear:
- Next-generation MRI, CT, and PET
- Genomic sequencing by the Tempus platform – they analyze the tumor’s DNA to select targeted therapy
- Referring patients for proton therapy (they don’t provide it on-site, but have established pathways)
- Eligibility for CAR-T treatment – these cellular immunotherapies
- Participation in phase I-III clinical trials through the global Cleveland Clinic network
This Tempus platform truly changes the approach. You take a tumor sample, sequence it, see what mutations are present, and only then decide on the medication. You’re not shooting in the dark.
Treatment model
I’ve already mentioned these Monday meetings—they’re called “tumour boards.” The entire multidisciplinary team sits down and discusses a single patient. The “patient-first” approach might sound like a marketing slogan, but here you can genuinely see the difference. Psycho-oncologists are involved from the very beginning, not just when someone breaks down after chemo.
Precision medicine, immunotherapy, targeted therapies—all of this is tailored individually. Two patients with the same type of cancer might receive completely different protocols because their tumors have different molecular profiles.
Outcomes and patient experience
The data speaks for itself. Patient satisfaction is around 95%. Five-year survival rates for selected cancers reach 85% or higher—clearly above the UK average. Over 50,000 outpatient visits annually, with growth of about 20% year on year. I’m not sharing this to boast—this is simply the result of our entire approach.
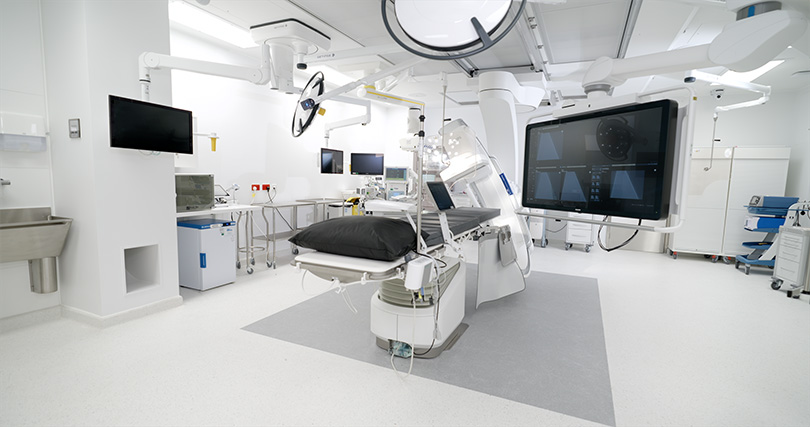
Let’s take an example: a man with early-stage prostate cancer. Rapid diagnostics—biopsy plus MRI. Genomic analysis of the tumor. A multidisciplinary team decides on the procedure. Surgery with the da Vinci Xi robot, post-operative check-ups, ongoing monitoring. From the first appointment to the procedure, it’s often just a matter of weeks, not months. Then, long-term follow-up and, if needed, additional therapy.
How to benefit from this and what’s next – the perspective of a Polish patient
You saw a post online about the “new Cleveland Clinic oncology center in London” and you’re wondering if this could be your chance for faster treatment. It’s understandable—Poland’s healthcare system can be overloaded, specialist wait times are getting longer, and when it comes to cancer, time is of the essence. But before you buy a ticket, it’s worth pausing and checking a few things.
Start by verifying the basic information on the hospital’s official website. Cleveland Clinic London has been around for a few years, but that doesn’t mean every social media post shares up-to-date facts. Sometimes people share old news, sometimes they mix up different facilities—you might see a date from three years ago and think it’s something new. Check the UK hospital registries, read patient reviews, but don’t rely solely on those from a Facebook group.
Here are some practical steps to help you make an informed decision:
- Book a consultation at a Polish specialist center – get a second opinion without the cost of travel
- Call your insurer and ask about reimbursement for treatment abroad (in most cases, you pay out of pocket).
- Calculate the total costs – therapy, flight, hotel, and sometimes family stay for several weeks
- Check if the center offers remote consultations before your trip
- Prepare medical documentation in English – results, histopathological descriptions
- Check the availability of appointments and waiting times, as it’s not always shorter than in Poland.

What might change in the coming years? Global hospital networks are expanding, artificial intelligence is supporting diagnostics, and precision medicine is becoming more accessible. For Polish patients, this could mean a wider range of options, but also more fragmented information and greater difficulty in determining where to seek help. Private centers in Europe will likely attract patients with advertising, but their quality doesn’t always match the price.

Cleveland Clinic London is a viable option for certain cases—especially complex ones that require extensive expertise. But it’s not for everyone, and not at any cost. Sometimes, choosing a center closer to home, in Warsaw or Kraków, where you have family nearby and don’t have to worry about language or distance, may be a better solution. The decision should be based on a conversation with your attending physician, reliable information, and an honest assessment of your own capabilities.
Marky
Luxury Reporter editorial team
Medicine





